
123 456 7890

123 456 7890
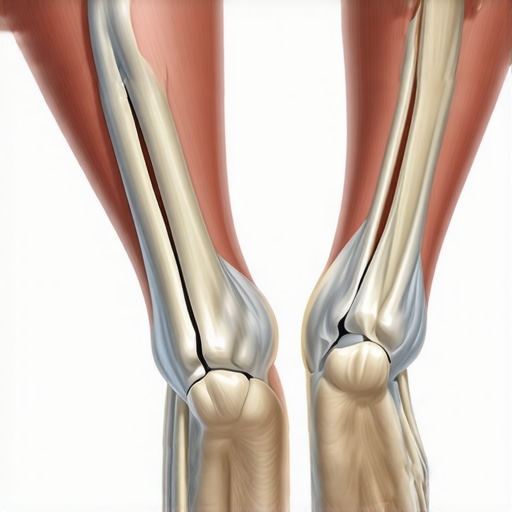
It was a morning like any other, but as I reached down to tie my shoelaces, a sharp twinge shot through my heel—something I had vaguely felt before but never paid much attention to. The dull ache was turning sharper, more persistent. Seriously, was I about to face another bout of plantar fasciitis that might drag on for months? I’ve been down this road before, and let me tell you, it’s not pretty. I realized that traditional treatments weren’t addressing the root cause—my foot’s mobility was slowly deteriorating, making it vulnerable. That moment sparked a lightbulb: what if the key to stopping plantar fasciitis in its tracks is fixing my foot’s mobility early on? Today, I want to share how small, focused mobility fixes can make a huge difference and might just prevent you from suffering the same fate. If you’re tired of endless heel pain, or WORSE, worried it’s coming back stronger, stick around. I’ll show you the proven strategies that helped me turn things around—fast. **How Improving Foot Mobility Can Save Your Future**Imagine feeling confident stepping out of bed without that familiar sting. Now, consider this: many people don’t realize that limited foot mobility often kicks off the cycle leading to plantar fasciitis. The problem isn’t just the pain; it’s the weakening of the tissues and joints that support your arch. The good news is, addressing this early can drastically reduce the chance of long-term damage—and even stop it before it really takes hold. As a sports rehab enthusiast, I’ve seen firsthand how tiny adjustments and targeted mobility drills can reverse the damage and prevent the nagging recurrence that plagues so many in 2026. Our feet are the foundation of movement—yet, they’re often neglected until pain becomes unbearable.But here’s where many go wrong. Early on, I made the mistake of just applying ice or popping pills, thinking that would fix the pain. Spoiler alert: it didn’t. Instead, I found that focusing on my foot’s range of motion, flexibility, and nerve flow was the real game changer. That’s when I discovered simple, effective mobility techniques that can be done in minutes daily. These strategies aren’t just theories—they’re backed by science. For example, nerve flossing drills targeting the nerves around the foot and ankle have been proven to accelerate healing by reducing tension (you can learn more about nerve flossing drills [here](https://motiontherapypro.com/3-nerve-flossing-drills-to-kill-sciatica-pain-fast-2026)). Incorporating these fixatives early on can save you months of pain and frustration, and ultimately, protect you from the debilitating cycle of chronic plantar fasciitis that often worsens in 2026.
Begin with gentle ankle circles, rotating your foot outward and inward for 30 seconds each direction. I remember my first attempt during a lazy Sunday morning; my ankle felt stiff, but I pushed through, and over a week, I noticed less heel discomfort. This simple movement increases joint lubrication and loosens tight tissues.
Use a towel to grip your toes, pulling them gently towards you for 15 seconds, then relax. I once neglected this step, leading to mild setbacks, but once I committed, I regained lost mobility quickly. These stretches reduce tension along the plantar fascia and improve flexibility.
Perform nerve flossing by gently toggling your toes while keeping your heel on the ground, aiming to move the nerve without causing pain. I followed a specific drill from this guide, which smoothed nerve pathways and alleviated lingering tightness in my foot, speeding recovery.

After increasing flexibility, add resistance band exercises that target the foot and ankle muscles. I cabled my foot against a resistance band for dorsiflexion and resisted toe presses; this built resilience and supported better arch support. Consistent strength training prevents tissues from overstretching again.
Set aside 5-10 minutes each morning for these drills; consistency trumps intensity. My early mornings were messy—forgetting steps and rushing—but routine proved effective in maintaining progress, preventing flare-ups, and ensuring ongoing foot health.
Many assume that quick fixes like spinal adjustments or stretching alone are enough to resolve persistent back pain or sports injuries. However, in my experience working with athletes and patients, the truth is far more complex. A common misconception is that targeting symptoms directly will lead to lasting relief, but this often neglects the underlying neuromuscular coordination and tissue health. For instance, countless individuals rely solely on chiropractic adjustments, believing they correct the root problem, yet studies reveal that without addressing movement patterns and nerve tension, relief is often temporary (see here). This is where many fall into the trap of superficial treatment. The real nuance lies in integrating detailed neuro-mobilization techniques, strengthening, and mobility work to optimize tissue function and nerve flow.
One advanced mistake is ignoring the role of nerve tension and mobility in recovery. A patient might receive adjustments, but if nerve impingement persists, pain returns quickly—highlighting how neurodynamics contribute to long-term healing. The concept of nerve flossing, for example, is often underrated (learn more here). By systematically releasing nerve restrictions, you can accelerate healing and prevent re-injury.
It’s tempting to believe that spinal manipulations remove all pain, but scientific reviews point out that adjustments mainly improve joint mobility and reduce immediate discomfort. Truly effective rehabilitation addresses muscle imbalances, tissue quality, and neural tension. Neglecting this multi-layered approach is a common oversight that hampers progress. Incorporating functional movement assessments, stability drills, and nerve mobility routines makes all the difference in sustaining improvement.
Certainly, the key lies in understanding that pain relief is just one piece of the puzzle. Advanced practitioners focus on restoring optimal neuromuscular communication, tissue resilience, and movement patterns. This holistic view prevents the pain from lurking back unexpectedly. So, if you’ve been relying solely on adjustments or stretching, consider whether you’re missing the deeper, often hidden, triggers of your pain. Would you like to explore these advanced strategies? Check out more about how chiropractic techniques can be combined with movement therapy for faster results.
Have you ever fallen into this trap? Let me know in the comments.
When it comes to sustaining the benefits of your sports rehab or chiropractic treatments, having the right tools and habits in place can make all the difference. Personally, I prioritize specific equipment and methods that not only enhance recovery but also empower long-term maintenance.
One essential tool I recommend is a set of resistance bands, particularly loop bands designed for ankle and foot exercises. These are invaluable for performing targeted mobility drills, like dorsiflexion and toe strengthening routines, which I do daily. Their portability allows me to maintain consistency outside the clinic or gym, ensuring ongoing tissue resilience.
Another device I swear by is a foam roller, especially for my calves and plantar fascia. Regular self-myofascial release helps prevent tissue tightness from creeping back in, which is crucial for avoiding flare-ups. I find that incorporating targeted rolling sessions post-exercise facilitates better circulation and tissue recovery, leading to more durable results.
Beyond physical tools, digital solutions like movement tracking apps can be game-changers. I utilize apps that monitor mobility ranges and symptom flare-ups, enabling me to adjust my routines proactively. This data-driven approach helps identify early signs of regression, so I can intervene before pain or dysfunction re-emerge.
Looking ahead, the trend is moving towards AI-driven platforms that analyze your movement patterns and suggest personalized exercises. This personalized feedback loop will become standard for proactive back health management, much like advanced sports analytics have transformed performance tracking.
Consistency remains the cornerstone of long-term success. Integrating brief but daily mobility and strengthening routines—like nerve flossing drills, which I personally do using guidance from this resource—ensures your tissues and nerves stay flexible and healthy. It’s tempting to think once you’re healed, the work is done. However, ongoing vigilance prevents re-injury and keeps your back pain at bay.
Maintaining your hard-won progress involves periodic check-ins, just like with any elite training regimen. Scheduling regular self-assessment sessions using apps or even simple flexibility tests can alert you when your mobility declines. Pair this with periodic visits to a practitioner for assessments, perhaps consulting about integrating new tools like the latest mobility devices I explored in 2026, found here. This proactive approach helps keep your back and nerves in top shape for the long haul.
Remember, combining physical tools like resistance bands and foam rollers with smart tracking creates a robust system to preserve mobility and prevent setbacks. Try integrating one new mobility tool or tracking method into your routine this week—your back will thank you!
One of the most eye-opening lessons I learned was that quick fixes and superficial treatments often only mask the pain, leaving underlying issues unaddressed. I’ve realized that true progress requires a deep understanding of movement patterns and neural health, not just symptom relief. This shift in perspective transformed my approach, helping me avoid recurring setbacks and achieve sustainable results.
Early in my journey, I underestimated how interconnected the nervous system, muscles, and connective tissues are. Recognizing that nerve tension, tissue quality, and joint mobility all play a role in pain meant I could tailor my rehab more effectively. This holistic view has been key to preventing the cycle of flare-ups that seemed inevitable before.
Over time, I’ve curated a toolkit that makes a real difference, including targeted resilience drills and smart tracking apps. Resources like nerve flossing drills have been game-changers, speeding recovery and reducing nerve-related discomfort. Incorporating resistance bands and foam rollers into my routine gives me the flexibility to maintain progress independently, even on busy days.
The path to pain-free movement isn’t a straight line, but every intentional step counts. By prioritizing mobility, neural health, and consistency, you’re investing in a future where pain no longer controls your life. Remember, the effort you put in today shapes your ability to move freely tomorrow. Ready to take action? Share your experiences below, and let’s support each other’s journey toward lasting relief.
Leave a Reply