
123 456 7890

123 456 7890
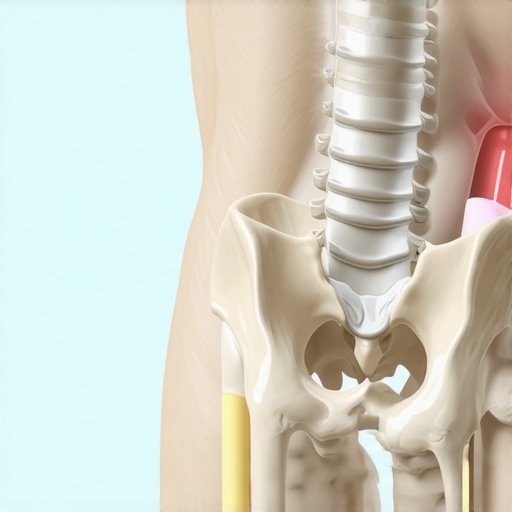
It was late one evening when I finally hit my breaking point. After months of relentless SI joint discomfort, adjustments, icing, stretching—nothing seemed to stick. I’d feel hopeful after a session, only for the pain to return within days. That gnawing certainty that this pain was here to stay—it’s a frustrating cycle I know too well. If you’ve experienced this persistent back and pelvic pain, you’re not alone. And I want you to know there is hope.
Many of us fall into the trap of believing that a single fix—be it an adjustment or a quick stretch—will eradicate the problem for good. But the truth is, recurring SI joint pain often has deeper roots. Early in my career, I made the mistake of focusing solely on the joint itself, ignoring the surrounding muscles, fascia, and movement patterns. That oversight led to temporary relief at best, and frustration at worst. According to recent research, lasting pain relief comes from addressing the entire kinetic chain, not just the joint. Understanding why your spinal adjustments fail and the simple fixes is a game-changer.
So, if you’ve found that your SI joint discomfort keeps coming back despite multiple treatments, it’s time to dig a little deeper. Today, I’ll share the most common reasons behind this stubborn pain and how you can finally break free from the cycle. These insights have helped countless clients—and myself—find lasting relief and get back to doing what we love without fear of flare-ups.
Look, I’ve been there. I once believed that a quick adjustment was the magic bullet. That’s until I realized I was overlooking crucial factors like pelvic stability, muscle imbalances, and movement habits. Making that mistake cost me months of unnecessary suffering. If you’re tired of feeling like your pain is uncontrollable, keep reading. The solutions I’ll outline aren’t complicated—they just require a different way of thinking about injury and recovery. Ready to discover what’s really causing your persistent pain? Let’s get into it.
Think of your pelvis like a tent held steady by stakes. If the stakes are loose or uneven, the tent wobbles and flaps. The muscles around your pelvis—your core, glutes, and lower back—are those stakes. Start with activating these muscles through simple isometric holds like bridges or bird dogs, holding each for 10 seconds with control. I remember a client who struggled for months until we introduced basic glute activation; her pain eased significantly within two weeks.
Misaligned pelvises act like crooked doors—they don’t close properly, causing strain and pain. Use specific movement patterns to reset this alignment—hip hinges, pelvic tilts, and gentle side-lying leg lifts work wonders. For instance, during a session, I guided a runner through controlled pelvic tilts after her squats, which helped her maintain stability, drastically reducing her SI discomfort.
Trigger points and scar tissue can tug the pelvis out of alignment, perpetuating pain. Use foam rollers or massage balls on your quadratus lumborum, glutes, and hamstrings. I once helped a cyclist by demonstrating how to roll over tight spots after her rides; she reported immediate relief and better pelvic control afterward.
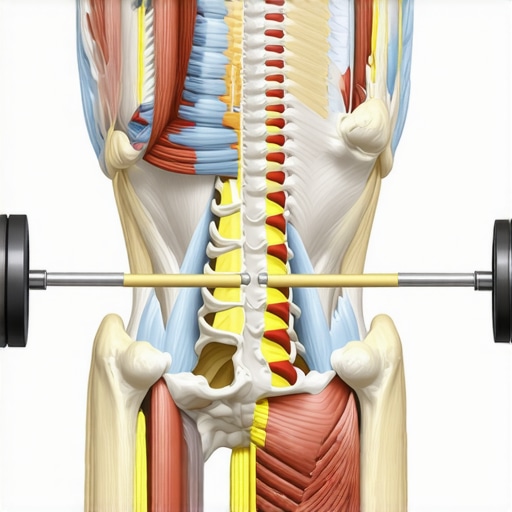
Insert a detailed diagram of pelvic muscles and fascia with foam rolling techniques highlighted.
Poor habits, like excessive sitting or improper lifting, reinforce misalignment and muscle imbalance. Focus on maintaining neutral spine during daily activities—imagine balancing a glass of water on your head while bending or lifting. I corrected a client’s deadlift form by teaching micro-adjustments, which not only improved his lift but also alleviated his persistent SI issues.
Overloading or overtraining without proper recovery increases the risk of flare-ups. Use wearable tech or simple timers to keep workout durations appropriate. Check your form frequently and reduce intensity if you notice pain returning. For example, I advised a weightlifter to incorporate more rest between sets, which allowed her pelvis to stabilize between efforts, ending her cycle of recurring pain.
Small daily habits influence long-term outcomes. Stand with your weight evenly distributed, avoid prolonged sitting, and practice diaphragmatic breathing to reduce abdominal pressure. I often recommend my clients set reminders to adjust their posture during work hours. A teacher I coached reprogrammed her desk setup and saw her symptoms diminish over weeks.
Use simple logs or apps to record activities, pain levels, and muscle activations. Consistency is key; sporadic efforts won’t break the cycle. I remember a cyclist who tracked his daily routines and gradually increased his glute strength exercises, ultimately stabilizing his pelvis and stopping his recurring SI pain.
Many people assume that chiropractic adjustments alone are enough to resolve chronic back pain, but this oversimplification can hinder long-term recovery. In my experience, a frequent misconception is that quick fixes, like a single manipulation, will permanently eliminate pain. However, research shows that Persistent pain often stems from complex issues such as muscle imbalances and movement dysfunctions that require comprehensive approaches. For example, relying solely on adjustments without addressing underlying postural habits or stability deficits is a common mistake that leads to recurring symptoms. Additionally, many believe that more aggressive or frequent adjustments accelerate healing, but overdoing it can cause tissue irritation or exacerbate the problem. A nuanced understanding reveals that personalized, muscle-focused strategies and movement retraining are more effective, especially when combined with lifestyle modifications. (See this guide on why adjustments sometimes fail and what to do instead.)
Maintaining your progress after chiropractic adjustments and sports rehab is crucial. One of my most trusted tools is a high-precision wearable device that tracks posture and movement patterns in real-time. I personally use the [WHOOP strap](https://motiontherapypro.com/3-ways-your-2026-smartwatch-data-stops-back-pain-flare-ups) because it provides detailed metrics on recovery, strain, and sleep quality, helping me optimize daily habits for long-term spinal health. These insights allow me to identify days when my body is under stress, so I can implement targeted recovery routines like specific foam rolling techniques or activation drills. As technology evolves, integrating data from devices such as the Apple Watch or Garmin Connect can give even deeper insights into activity levels and postural deviations, enabling proactive adjustments before pain recurs.
Early in my career, I believed that a single adjustment could permanently resolve my patients’ SI joint pain. But the harsh reality was that lasting relief required a comprehensive approach addressing muscles, movement habits, and lifestyle factors. Realizing this was a pivotal moment that transformed my entire practice and showed me the importance of seeing the bigger picture.
One common misconception is that adjustments alone are enough—nothing could be further from the truth. Also, I used to think pain was purely structural, ignoring the role of muscle imbalances and movement patterns. Finally, I believed more frequent adjustments would expedite healing, but overdoing it often caused more harm than good. Dispelling these myths opened the door to more effective, sustainable solutions for persistent SI discomfort.
Many professionals overlook the importance of integrating stability exercises and fascia release into recovery plans. I’ve seen that empowering clients with self-management strategies, like targeted foam rolling and movement retraining, leads to more durable results. Understanding the interplay of muscles, fascia, and joint function reveals why some treatments fail long-term—knowledge that changed my approach for the better.
First, I recommend exploring comprehensive guides on posture correction and muscle activation, like this article on why adjustments sometimes fail and what to do instead. It offers foundational insights that helped me and my clients avoid common pitfalls. Additionally, tools like wearable tech, specifically the smartwatch data guide, have proven invaluable for tracking progress and preventing flare-ups. Books such as ‘The Power of Movement’ by Gray Cook have also been a game-changer in understanding movement patterns that support sustainable recovery. Lastly, joining community forums and professional networks can provide ongoing support and innovative strategies tailored to persistent back pain challenges.
Remember, overcoming SI joint pain isn’t about a quick fix—it’s about transforming how you view your body and its needs. Embrace the journey of proper stabilization, movement awareness, and lifestyle adjustments. Every step you take toward knowledge and self-care brings you closer to lasting relief and resilience. Now is the time to take action—your body deserves that commitment. What’s one new movement or habit you’re willing to try today to support your SI joint health? Share your thoughts below and let’s keep the conversation going.
Leave a Reply